Getting and keeping patients healthy is the primary goal of every healthcare facility, but that goal can be hard to achieve. When it comes to high-level disinfection and disinfectants (HLDs), there are so many options on the table that it can be difficult to figure out and stay current on what best practices are. In recent years the development of single-use HLDs has introduced a new question: is single-use a better option than reusable? Reusable disinfectants have been the standard for decades, so one must determine whether single-use disinfectants are actually better at mitigating risk for patients.
According to Drs. William Rutala and David Weber, "Semicritical items represent the greatest risk of disease transmission as far more health care associated infections have been caused by semicritical items than critical or noncritical items." That being the case, it is important for healthcare providers to ensure that they employ best practices to keep patients healthy. In order to determine what best practices are, we will review the process of high-level disinfection and evaluate possible issues when using either single-use or reusable HLDs to high-level disinfect a transesophageal echocardiogram ultrasound (TEE) probe.
To high-level disinfect a point of use cleaned, enzymatically cleaned, and properly dried TEE probe with reusable HLD, one must first ensure that the HLD has not expired. Then, the HLD must be MRC tested using test strips which must be brand-specific (the test strips, themselves, must also be tested prior). The directions for solution temperature, time for testing, and desired results vary between brands. If the HLD has passed testing, then it can be used for high-level disinfection. It is important to exactly follow the HLD's instructions for use to determine soak time and temperature as this affects whether or not a probe has been disinfected. The disinfection process may take anywhere between 8-45 minutes depending on the chemical used and contact temperature. One must not leave the probe unattended during this period if manually disinfecting to prevent the risk of damage due to oversoaking. After this, the probe can be rinsed, dried, and stored.
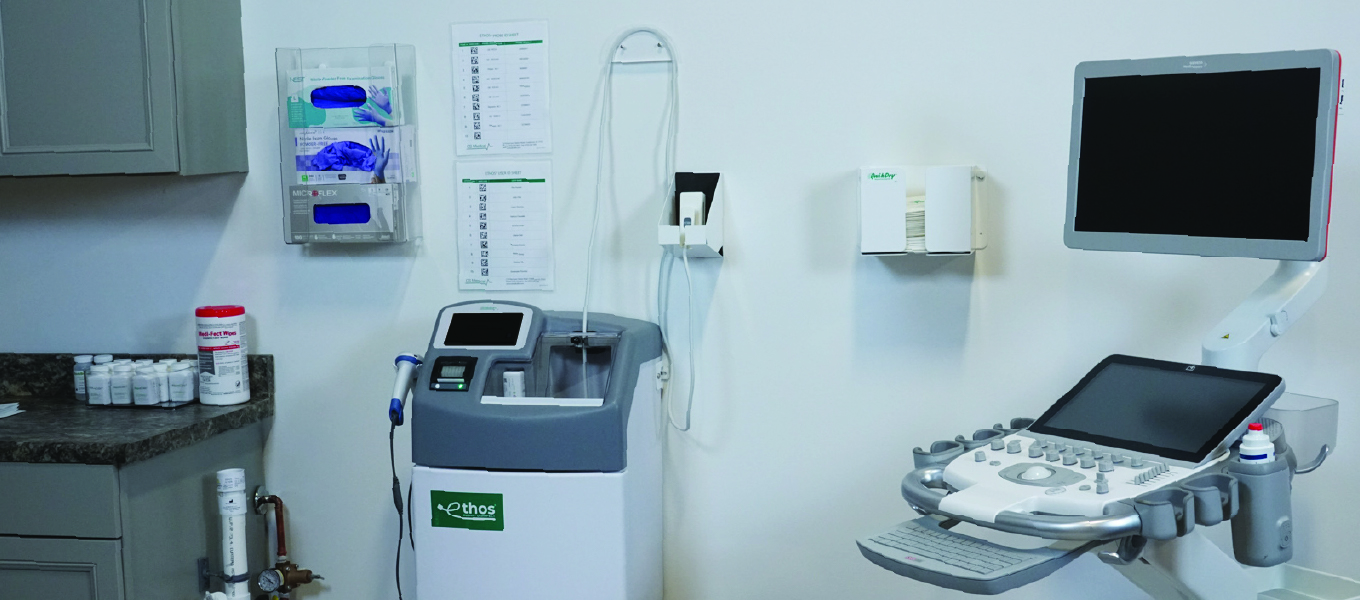
High-level disinfecting when employing single-use HLD is a very different process. One must simply place the fully cleaned and dried TEE probe into the automated disinfecting device's reservoir and load a pint-sized HLD into the machine. High-level disinfection takes 5 minutes followed by automated rinsing, totaling 17 minutes for the entire cycle, during which the probe may be left unattended. At this point, the probe can be dried and stored.
Whether a facility chooses single-use or reusable HLDs will impact staff in significant ways. To begin with, staff must be trained to reprocess probes. As the process utilizing reusable HLDs is more involved than for single-use HLDs, training takes up more time and leaves far more room for error. Reusable HLDs require MRC testing before every use, taking up valuable time. Reusable HLDs also often require more staff attention during the disinfection process, especially if the probe is being manually reprocessed and cannot be left unattended during the 8-45 minute wait time. If staff is not on hand to supervise or has not been properly trained, contamination of the disinfectant is possible and poses a serious risk. All this extra time required by reusable HLDs comes at a price; time is money and labor is not free. Additionally, a pint-sized bottle (1lb) of single-use HLD is easier for staff to handle than more cumbersome gallon-sized jugs (8-9lbs) of reusable HLDs, potentially resulting in fewer spills.
Single-use HLDs minimize staff's exposure to the harsh chemicals in HLDs, keeping them healthy. If manually reprocessing probes, staff members are exposed to basins full of HLD and their vapors for long stretches of time. Even when using an automated high-level disinfector, staff members have to open each gallon of HLD and hook it up to the appropriate ports. When the time comes to change the HLD, staff must remove the HLD, neutralize the solution, and dispose of it. Single-use disinfectants, on the other hand, have a foil seal that is punctured by the automated disinfector. Before staff members remove the bottle, the machine automatically rinses it, making it safe to handle and recycle.
A facility's choice of HLD also has a huge impact on patients. Semicritical items represent a threat to the wellbeing of patients when not properly reprocessed. MRC testing reusable HLDs is complex and requires that staff members have a thorough understanding of the chemistry and follow instructions to the letter every single time, without exception. That being the case, Rutala and Weber report that, "… audits have shown that personnel do not consistently adhere to guidelines on reprocessing and that outbreaks of infection continue to occur." This puts patients at risk for contracting healthcare-associated infections (HAIs), going against everything the healthcare industry strives for. Single-use HLDs mitigate this risk by removing room for human error, ensuring the proper amount and potency of HLD every time.
Finally, one must consider how choice of single-use or reusable HLD financially influences a facility. The most obvious difference between single-use and reusable HLDs is their price up front. Reusable disinfectants often cost around $50.00 per bottle and can be used several times; there are claims that a single bottle will retain MRC through forty or more cycles. Conversely, single-use disinfectants cost about $7.00 per bottle and can only be used once.
However, one must also account for the cost of test strips required for reusable disinfectants. On average, a bottle of test strips can cost anywhere from $80.00-$125.00. Most major brands require six test strips to be used to initially validate the actual test strips, a process that takes valuable time. Then, a test strip must be used and properly read before each use of the reusable HLD, which also takes time. These reading are not always straightforward, though, which can cause confusion and lead to improper readings and risky conditions for patients.
As a result of the complexity of properly utilizing reusable HLDs, a facility must factor in the higher risk associated with reusable HLDs. Single-use HLDs help mitigate that risk significantly by removing much of the possibility for human error. Reusable HLDs leave a facility financially liable in the case of human error or negligence. According to the CDC, "By law, all applicable label instructions on EPA-registered products must be followed. If the user selects exposure conditions that differ from those on the EPA-registered product label, the user assumes liability for any injuries resulting from off-label use..." If a staff member is having a hard day, they are more likely to make mistakes or cut corners. Unfortunately, everyone has bad days, so the chances are high that mistakes will happen and a facility will have to pay the price with their pocketbook and reputation while a patient may pay with their health or even their life.
All in all, when determining whether a facility will employ reusable or single-use HLDs, all factors must be taken into consideration. Single-use HLDs simplify reprocessing for staff members, keep occupational exposure down, help provide the best outcomes for patients, can keep operating costs low, and assist a facility in mitigating risk. Single-use HLDs are a great way to help ensure that a facility is using best practices when reprocessing their semicritical devices. After a review of all the available information, it would seem that a facility has only to gain by switching over to single-use HLDs.
| Reuseable HLD | Single-Use HLD | |
|---|---|---|
| Time needed to disinfect | 8-45 minutes | 5 minutes |
| Training needed | Extensive (validating test strips, testing solution for MRC, determining time and temperature necessary, etc.) | Basic (operating the automated disinfector) |
| Staff safety | Increased exposure to HLDs | No exposure to HLDs |
| Patient safety | Patient is at greater risk for HAI (dependent on perfect disinfection by staff every time) | Patient risk for contracting HAI is minimal |
| Cost of HLD | ~$50.00/gallon | ~$7.00/pint |
| Cost of test strips | ~$100.00/bottle | N/A |
| Risk | Plenty of room for human error (mistakes in test strips, time required, constant handling of probes, spills, etc.) | Minimized room for human error (the automated disinfector deals with all those factors) |